Analysis / Statistics (4)
Absolutely necessary technical services. No consent necessary.
Meta Pixel (via Matomo TagManager)
Meta Platforms Ireland Ltd., Ireland
When accessing some sub-services of our website, additional personal services are processed. Processed data categories: technical connection data of the server access (IP address, date, time, requested page, browser information)data about the use of the website and the logging of clicks on individual elements. Purpose of processing: Anonymization and creation of statistics, analysis of user behavior and content optimization. The legal basis for processing: Your consent according to Art. 6 (1) a GDPR. Data is transmitted: to the data controller Meta Platforms Ireland Ltd., 4 Grand Canal Square, Grand Canal Harbour, Dublin 2, Ireland. The legal basis for the data transfer to Meta Platforms Ireland Ltd. is Your consent according to Art. 6 (1) a GDPR. This may also mean a transfer of personal data to a country outside the European Union. The data is transferred to the USA on the basis of Art. 45 GDPR in conjunction with the European Commission's adequacy decision C(2023) 4745, since the data recipient has committed to comply with the data processing principles of the Data Privacy Framework (DPF).
Hotjar (via Matomo TagManager)
Hotjar Limited, Malta
Personal data is processed when you visit this website. Processed data categories: technical connection data of the server access (IP address, date, time, requested page, browser information)data about the use of the website and the logging of clicks on individual elements. Purpose of processing: Anonymization and creation of statistics, analysis of user behavior and content optimization. The legal basis for processing: Your consent according to Art. 6 (1) a GDPR. Data is transmitted: to the data processor Hotjar Limited, Level 5, Dragonara Business Centre, Dragonara Road, Paceville St Julian's STJ 3141, Malta. This may also mean a transfer of personal data to a country outside the European Union. The data is transmitted on the basis of your consent in accordance with Art. 6 Para. 1 lit a in conjunction with Art. 49 Para. 1 lit a GDPR. You were informed before you gave your consent that the USA does not have a level of data protection that corresponds to the standards of the EU. In particular, US secret services can access your data without you being informed and without you being able to take legal action against it.
ActiveCampaign (via Matomo TagManager)
ActiveCampaign, LLC., USA
Personal data is processed when you visit this website. Processed data categories: data for creating usage statistics. Purpose of processing: Anonymization and creation of statistics and analysis of user behavior. The legal basis for processing: Your consent according to Art. 6 (1) a GDPR. Data is transmitted: to the data controller ActiveCampaign, 1 North Dearborn Street, 5th floor Chicago, IL 60602 Chicago, USA. The legal basis for the data transfer to ActiveCampaign is Your consent according to Art. 6 (1) a GDPR.
Cloudflare Webtracking (via Matomo TagManager)
Cloudflare, Inc,
Personal data is processed when you visit this website. Processed data categories: data for creating usage statistics. Purpose of processing: Anonymization and creation of statistics and analysis of user behavior. The legal basis for processing: Your consent according to Art. 6 (1) a GDPR. Data is transmitted: to the data controller Cloudflare Webtracking, , . The legal basis for the data transfer to Cloudflare Webtracking is Your consent according to Art. 6 (1) a GDPR.
Targeting / Profiling / Advertising (7)
Personalized advertising outside our website
Bing Ads (Microsoft UET) (via Matomo TagManager)
Microsoft Ireland Operations Limited, Ireland
Personal data is processed when you visit this website. Processed data categories: data about the use of the website and the logging of clicks on individual elements. Purpose of processing: analysis of user behavior, Analysis of the effect of online marketing measures and Selection of online advertising on other platforms, which are automatically selected using real-time bidding based on user behavior. The legal basis for processing: Your consent according to Art. 6 (1) a GDPR. Data is transmitted: to the data controller Microsoft Ireland Operations Limited, One Microsoft Place South County Business Park, Leopardstown Dublin, 18 D18 P521, Ireland. The legal basis for the data transfer to Microsoft Ireland Operations Limited is Your consent according to Art. 6 (1) a GDPR. This may also mean a transfer of personal data to a country outside the European Union. The data is transferred to the USA on the basis of Art. 45 GDPR in conjunction with the European Commission's adequacy decision C(2023) 4745, since the data recipient has committed to comply with the data processing principles of the Data Privacy Framework (DPF).
Meta Pixel (via Matomo TagManager)
Meta Platforms Ireland Ltd., Ireland
Personal data is processed when you visit this website. Processed data categories: data about the use of the website and the logging of clicks on individual elements. Purpose of processing: analysis of user behavior, Analysis of the effect of online marketing measures and Selection of online advertising on other platforms, which are automatically selected using real-time bidding based on user behavior. The legal basis for processing: Your consent according to Art. 6 (1) a GDPR. Data is transmitted: to the data controller Meta Platforms Ireland Ltd., 4 Grand Canal Square, Grand Canal Harbour, Dublin 2, Ireland. The legal basis for the data transfer to Meta Platforms Ireland Ltd. is Your consent according to Art. 6 (1) a GDPR. This may also mean a transfer of personal data to a country outside the European Union. The data is transferred to the USA on the basis of Art. 45 GDPR in conjunction with the European Commission's adequacy decision C(2023) 4745, since the data recipient has committed to comply with the data processing principles of the Data Privacy Framework (DPF).
Google GTag (via Matomo TagManager)
Google Ireland Limited, Ireland
Personal data is processed when you visit this website. Processed data categories: data about the use of the website and the logging of clicks on individual elements. Purpose of processing: analysis of user behavior, Analysis of the effect of online marketing measures and Selection of online advertising on other platforms, which are automatically selected using real-time bidding based on user behavior. The legal basis for processing: Your consent according to Art. 6 (1) a GDPR. Data is transmitted: to the data controller Google Ireland Limited, Gordon House, Barrow Street, Dublin 4, Ireland. The legal basis for the data transfer to Google Ireland Limited is Your consent according to Art. 6 (1) a GDPR. This may also mean a transfer of personal data to a country outside the European Union. The data is transferred to the USA on the basis of Art. 45 GDPR in conjunction with the European Commission's adequacy decision C(2023) 4745, since the data recipient has committed to comply with the data processing principles of the Data Privacy Framework (DPF). The privacy policy of Google Ireland Limited:
https://business.safety.google/privacy/.
LinkedIn Pixel (via Matomo TagManager)
LinkedIn Ireland Unlimited Company, Ireland
Personal data is processed when you visit this website. Processed data categories: data about the use of the website and the logging of clicks on individual elements. Purpose of processing: analysis of user behavior, Analysis of the effect of online marketing measures and Selection of online advertising on other platforms, which are automatically selected using real-time bidding based on user behavior. The legal basis for processing: Your consent according to Art. 6 (1) a GDPR. Data is transmitted: to the data controller LinkedIn Ireland Unlimited Company, Wilton Place, Dublin, D02 X527, Ireland. The legal basis for the data transfer to LinkedIn Ireland Unlimited Company is Your consent according to Art. 6 (1) a GDPR. This may also mean a transfer of personal data to a country outside the European Union. The data is transferred to the USA on the basis of Art. 45 GDPR in conjunction with the European Commission's adequacy decision C(2023) 4745, since the data recipient has committed to comply with the data processing principles of the Data Privacy Framework (DPF).
TikTok Pixel (via Matomo TagManager)
TikTok Technology Limited, Ireland
Personal data is processed when you visit this website. Processed data categories: data about the use of the website and the logging of clicks on individual elements. Purpose of processing: analysis of user behavior, Analysis of the effect of online marketing measures and Selection of online advertising on other platforms, which are automatically selected using real-time bidding based on user behavior. The legal basis for processing: Your consent according to Art. 6 (1) a GDPR. Data is transmitted: to the data controller TikTok Technology Limited, 10 Earlsfort Terrace, Dublin, D02 T380, Ireland. The legal basis for the data transfer to TikTok Technology Limited is Your consent according to Art. 6 (1) a GDPR. This may also mean a transfer of personal data to a country outside the European Union. The data is transmitted on the basis of your consent in accordance with Art. 6 Para. 1 lit a in conjunction with Art. 49 Para. 1 lit a GDPR. To contact the data protection officer by email TikTok Technology Limited:
https://www.tiktok.com/legal/report/DPO. The privacy policy of TikTok Technology Limited:
https://www.tiktok.com/legal/privacy-policy-eea?lang=de.
Spotify (via Matomo TagManager)
Spotify AB, Sweden
Personal data is processed when you visit this website. Processed data categories: data about the use of the website and the logging of clicks on individual elements. Purpose of processing: Anonymization and creation of statistics, Selection of online advertising on other platforms, which are automatically selected using real-time bidding based on user behavior and analysis of user behavior. The legal basis for processing: Your consent according to Art. 6 (1) a GDPR. Data is transmitted: to the data controller Spotify, Regeringsgatan 19, 111 53 Stockholm, Sweden. The legal basis for the data transfer to Spotify is Your consent according to Art. 6 (1) a GDPR.
Pinterest Profiling (via Matomo TagManager)
Pinterest Europe Ltd., Ireland
Personal data is processed when you visit this website. Processed data categories: data about the use of the website and the logging of clicks on individual elements. Purpose of processing: analysis of user behavior, Analysis of the effect of online marketing measures and Selection of online advertising on other platforms, which are automatically selected using real-time bidding based on user behavior. The legal basis for processing: Your consent according to Art. 6 (1) a GDPR. Data is transmitted: to the data controller Pinterest Europe Ltd., Palmerston House, 2nd Floor, Fenian Street, Dublin 2, Ireland. The legal basis for the data transfer to Pinterest Europe Ltd. is Your consent according to Art. 6 (1) a GDPR. This may also mean a transfer of personal data to a country outside the European Union. The data is transmitted on the basis of your consent in accordance with Art. 6 Para. 1 lit a in conjunction with Art. 49 Para. 1 lit a GDPR. You were informed before you gave your consent that the USA does not have a level of data protection that corresponds to the standards of the EU. In particular, US secret services can access your data without you being informed and without you being able to take legal action against it. To contact the data protection officer by email Pinterest Europe Ltd.:
https://help.pinterest.com/de/data-protection-officer-contact-form. The privacy policy of Pinterest Europe Ltd.:
https://policy.pinterest.com/de/privacy-policy.
Integration of additional information
YouTube
Google Ireland Limited, Ireland
When accessing some sub-services of our website, additional personal services are processed. Processed data categories: technical connection data of the server access (IP address, date, time, requested page, browser information)data for creating usage statistics. Purpose of processing: Delivery of content provided by third parties, Selection of online advertising on other platforms, which are automatically selected using real-time bidding based on user behavior and transmission and display of video content. The legal basis for processing: Your consent according to Art. 6 (1) a GDPR. Data is transmitted: as joint controllers for Google Ireland Limited, Gordon House, Barrow Street, Dublin 4, Ireland. This may also mean a transfer of personal data to a country outside the European Union. The data is transferred to the USA on the basis of Art. 45 GDPR in conjunction with the European Commission's adequacy decision C(2023) 4745, since the data recipient has committed to comply with the data processing principles of the Data Privacy Framework (DPF).
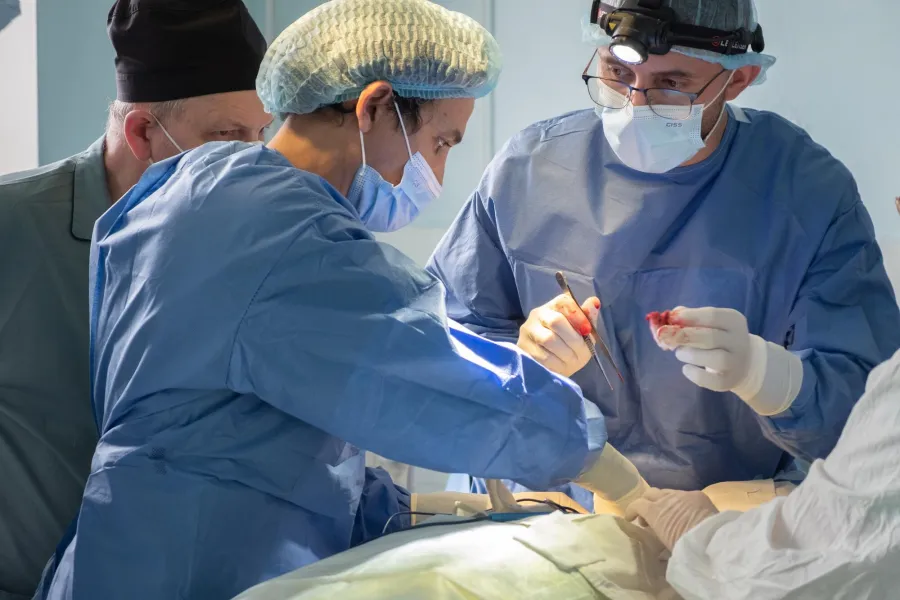
 Right now I’m based at the main hospital in Kostiantynivka. The frontline moves and we’ve been close to it many times. Every day we hear the sound of artillery – both incoming and outgoing – and the sound of explosions on the outskirts of the city.
Right now I’m based at the main hospital in Kostiantynivka. The frontline moves and we’ve been close to it many times. Every day we hear the sound of artillery – both incoming and outgoing – and the sound of explosions on the outskirts of the city.